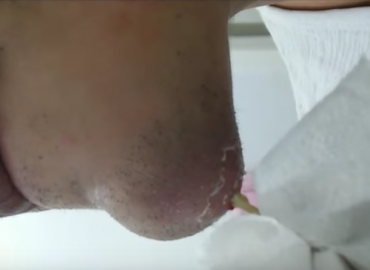
It is rarely a good idea to pop pimples, since doing so can cause scars or worsen your breakout. If you must pop a pimple, the best way to prevent damage is to use a needle. Alternatively, applying a wet rag can gently remove a whitehead. Using your hands to squeeze the pimple is not recommended, but can be done if the other methods seem too labor-intensive.
Determining Whether a Pimple Can Be Popped
Pop whitehead pimples. Whitehead pimples have usually been around for a few days, and they have a white tip where pus has collected underneath the skin. These pimples are easy to pop, and when treated with care they can be safely removed without spreading the infection or causing scarring.
Don’t pop new pimples. Pimples that have just appeared in the past day or two aren’t ready to pop yet. Wait until the whitehead appears at the tip of the blemish.
Don’t pop pimples that are big, red, or sore. This could worsen your pimple by sending bacteria deeper into your skin. Popping a pimple this big will almost definitely lead to a scar. Only a pimple with white pus is ready to pop.
Visit a dermatologist. Dermatologists can determine the best way to treat your acne. They can prescribe creams that will eliminate your pimples. There are also several procedures they can perform that can treat severe breakouts.
The most commonly prescribed dermatologist treatment is a topical cream, rubbed on the pimples, that will remove oil from the skin and kill acne-causing bacteria.
For red, swollen pimples an oral antibiotic, hormonal birth control, or isotretinoin might be prescribed.
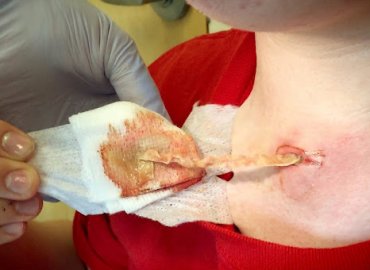
Large acne cysts can be removed by dermatologists through drainage and extraction, in which they remove the cyst and drain out the pus.
Your dermatologist can safely lance the pimple with a pin. This is a technique that should only be done by professionals.
Laser therapies and chemical peels can treat the underlying causes of acne, although they will not remove current cysts.
Limit pimples by washing regularly. Pimples are caused by sweat sitting on your face. Anytime you sweat, wash your face gently with lukewarm water to remove dirt and grime. Do not be harsh or scrub, just wash off sweat.
Scrubbing roughly can worsen acne.
Do not use rough cleaners, like astringents, toners, or exfoliants.
Prepping Your Hands and the Pimple
Wash your hands. This will prevent bacteria from spreading to your face. Wash thoroughly, especially underneath the nails, and use plenty of soap and warm water. You’ll want to avoid touching the pimple with your finger nails, but just in case you do, having them clean will reduce the likelihood of irritation and infection.
Consider using a fingernail brush to get dirt out from under your fingernails.
Cover your hands. Put on disposable gloves just before you’re ready to pop the pimple. Not only will this put a barrier between any remaining bacteria on your fingers (and in your fingernails) and your skin, but it will also prevent the sharp edges of your nails from impacting the pimple.
If you don’t have disposable gloves, you can cover your fingers with clean tissues.
Clean the skin surrounding the pimple with a face cleanser or rubbing alcohol. Apply cleanser to a cotton ball and spread it. When you pop the pimple, you’ll be opening the skin, creating a way for bacteria to enter. The pimple will heal faster if you don’t give bacteria a chance to settle in and create a new or worse infection.
Don’t scrub the area too hard, or you’ll irritate it further. Gently cleanse the area, rinse it with warm water, and pat it dry with a towel.
Popping a Pimple with a Pin
Sterilize a pin with fire. Use a match or lighter to heat up and sterilize the pin. Expose every bit of the pin to fire for several seconds to kill off any bacteria.
Allow the pin to cool. Give the pin at least a minute to cool down. It should not be painfully hot when you use it to pop your pimple.
Sterilize everything with rubbing alcohol. Apply rubbing alcohol to the pin, to your hands, and to the zit. Be sure that everything involved in the procedure is sanitized with rubbing alcohol.
Hold the pin parallel to your face. You do not want to point the pin toward your face. Instead, you should hold it along your face, so that when you poke your pimple it won’t penetrate anything but the very tip of the pimple.
Pierce the white tip of the zit. Do not touch anything but the white part of the zit. Penetrating the red part of the pimple will cause scarring. Instead, run the pin through the very tip of the pimple, so that it goes through one end and out the other.
Pull up with the pin. The pin should have penetrated the length of the white tip. Pull the pin out, away from your face, so that it ruptures the white tip when you remove the pin from the pimple.
Gently squeeze around the white top. Do not squeeze the white top itself. Instead, squeeze the perimeter of the pimple so that it pushes out the pus. Consider squeezing with a cotton swab to avoid doing additional damage to the skin.
Apply alcohol to the pimple. Use a cotton swab to rub the area down with alcohol and clean up bacteria. Apply a small amount of bacitracin ointment to the area.
PER CYST TEXT PER LINK
Distinguish between a sebaceous cyst and epidermoid cyst. An epidermoid cyst is more common than a sebaceous cyst. Each will have slightly different symptoms and will be treated just a little differently. Therefore, it is important that the cyst you have on your skin is diagnosed appropriately for effective treatment.
Both types of cysts are flesh-colored or white-yellow and have a smooth surface.
Epidermoid cysts are more common. These are slow growing and often painless. They don’t usually require treatment, unless they are causing pain or become infected.
Pilar cysts are composed primarily of keratin (the protein that makes up hair and nails) and form from the outer hair root sheath, typically on the head. A pilar cyst is often thought to be another term for a sebaceous cysts, but they are in fact different.
Sebaceous cysts are commonly found in the hair follicles on the head. They form inside the glands that secrete sebum, an oily substance that coats the hair. When these normal secretions are trapped, they develop into a pouch containing a cheese-like substance. They are commonly found in areas near the neck, upper back, and on the scalp. Sebaceous cysts are often confused with pilar or epidermoid cysts.
Distinguish between cysts in the breast and tumors. Cysts can be in one or both breasts. Without a mammogram or needle biopsy it is almost impossible to distinguish between the two different types of lumps in the breast. Symptoms of a breast cyst will include:
Smooth, easily movable lump with distinct edges
Pain or tenderness over the lump
Size and tenderness will increase just before your period starts
Size and tenderness will decrease when your period ends
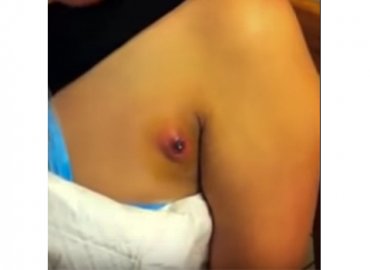
Understand cystic acne. Acne is a general term that describes a variety of different types of pimples, blackheads, pustules, whiteheads and cysts. Cystic acne are nodules that are red, raised, often 2–4 mm in size and nodular and are the most severe form of acne. The infection in a cystic acne is deeper than that in other pustules or whiteheads. Cystic acne is painful.
Identify a ganglion cyst. These are the most common types of lumps found on the hand and wrist. They are not cancerous and often harmless. Filled with fluid, they can quickly appear, disappear or change in size. They do not require treatment unless they interfere with function or are unacceptable in appearance.
Determine if pain is from a pilonidal cyst. In this condition there is a cyst, abscess or dimple that forms in the crease between the buttocks that runs from the lower end of the spine to the anus. It can be caused from wearing tight clothing, excess body hair, sitting for long periods of time or obesity. Symptoms can include pus from the area, tenderness over the cyst, or the skin may be warm, tender or swollen near the tailbone. Or there may not be any symptoms beside a pit or dimple at the base of the spine.
Distinguish a Bartholin gland cyst. These glands are located on either side of the vaginal opening to lubricate the vagina. When the gland becomes obstructed, a relatively painless swelling forms called a Bartholin’s cyst. If the cyst is not infected you may not notice it. An infection can occur in a matter of days causing tenderness, fever, discomfort walking, pain with intercourse, and a tender, painful lump near the vaginal opening.
See a doctor for swelling in the testicles. All testicular swelling must be diagnosed by a physician to determine the differences between a cyst, cancerous growth, hydrocele or infection in the testicles. A testicular cysts, also called a spermatocele or epididymal cyst, is typically a painless, fluid-filled, noncancerous sac in the scrotum above the testicles. T
Consider getting a second opinion if you are not satisfied with your physician’s diagnosis and treatment. Although most epidermoid and pilar cysts do not require treatment from a physician, if you do seek medical advice and are not satisfied with the results seek a second opinion. Most sebaceous and epidermoid cysts are straightforward, but there are other conditions that may mimic these cysts.
In a case study written in the Royal College of Surgeons of England, the authors presented two cases in which melanoma and a deep oral cavity were originally mistaken for a sebaceous cyst.
There are a variety of other infectious processes that may be mistaken for a sebaceous cyst, including boils, furuncles and carbuncles.
Treating a Cyst at Home
Treat uninfected epidermoid and sebaceous cysts at home. Signs of infection include the area becoming swollen, red, tender, or red and warm. If your home treatment for these cysts is not effective or if you experience symptoms, which indicate an infection, you should seek medical care from your physician.
If the cyst causes pain or discomfort with walking or intercourse, medical care is needed to treat the cyst.